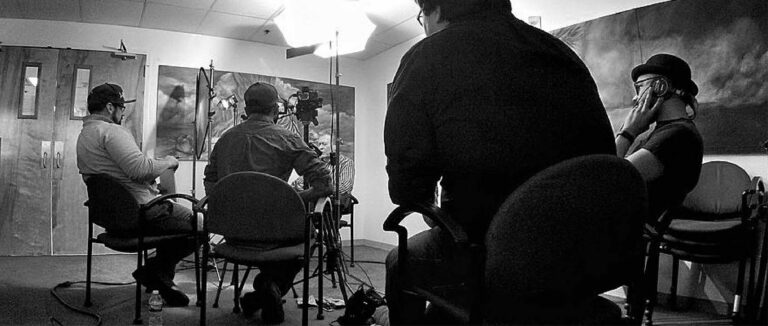Paula had been living with knee pain for years. The kind that takes things from you slowly. First it was the long walks. Then it was golf. Then it was the bike rides she used to take without thinking about it. By the time she sat down with us on camera, she’d already gotten the iovera treatment. She was back on the golf course. Back on her bike. When she talked about it, she didn’t talk about the device. She talked about the morning she woke up & realized the pain was gone.
That moment, a woman describing a morning, is what happens when a medical device company decides to tell a real story.
Not a product demo. Not a spec sheet on camera. A real person, sharing what actually changed.
We’ve spent years producing these kinds of films for medtech companies, & we’ve seen what happens when organizations invest in real human stories versus the alternative. The difference isn’t subtle. It shows up in how physicians respond, how sales teams perform, & how the market remembers the device years later.
The iovera Patient Stories: What Real Looks Like
When Pacira BioSciences asked us to produce patient story films for their iovera device, the brief could have gone in a predictable direction. Product features. Clinical data. Physician endorsements. All important. All necessary somewhere in the content mix.
But the films that ended up mattering most were the ones that started with a person, not a product.
Paula’s story was one. Mary Ellen’s was another. Mary Ellen’s arc was remarkable: she started as an iovera patient, experienced the results firsthand, & was so moved by her own recovery that she became a practitioner who now treats other patients with the same technology. She went from sitting in the chair to standing behind it.
You can’t script that. You can’t brainstorm it in a conference room. You find it by asking real patients what happened to them & listening with the camera rolling.
When those films went out to the sales team, the response was immediate. Reps reported that physicians watched the full videos in meetings, something that almost never happens with product content. The patient stories opened conversations that product decks couldn’t. Physicians saw their own patients in Paula & Mary Ellen. They felt something. That feeling became a conversation, & that conversation became a decision.
EXPAREL: Recovery Stories That Changed the Conversation
The EXPAREL work taught us something different about medical device storytelling. EXPAREL is a post-surgical pain management solution, which means the patient’s experience happens in one of the most vulnerable moments of their life: waking up after surgery.
Lea was facing ACL surgery. She was terrified. Not of the procedure itself, but of the recovery, the pain, the fog of heavy medication, the loss of control. When we filmed her story after her procedure, what she talked about wasn’t the product. She talked about waking up clear-headed. She talked about being present with her family in the hours after surgery instead of lost in a haze. She talked about a recovery that felt human.
Eric’s story had the same quality. A different procedure, a different person, but the same core experience: the surprise of waking up & feeling like yourself. Both stories carried weight not because they made claims about the product, but because they described experiences that any surgeon would want for their patients.
That’s the shift that happens when you commit to real storytelling. The product stops being the subject & becomes the reason the story is possible. The human experience moves to the center. The device is the supporting character that made the moment happen.
The PKD Documentary: When the Stakes Are Life & Death
Not every medical device story has a happy ending in the traditional sense. Sometimes the story is about living with uncertainty, making impossible decisions, & facing what’s coming with dignity.
We produced a documentary about a family facing polycystic kidney disease. Three siblings, all dealing with the same diagnosis. Kidney failure was part of their shared future, & each one was navigating it differently. One had already received a transplant. The others were in various stages of treatment & waiting.
This wasn’t a product story in the conventional sense. It was a story about the human reality that medical devices exist to address. The film didn’t sell anything. It built belief. It showed the audience, physicians, researchers, donors, & families, why the work matters. Why the research matters. Why every incremental improvement in treatment matters.
When a medical device company commits to telling stories like this, something shifts in how the organization is perceived. It goes from being a vendor to being an ally. From selling a product to serving a mission. That shift doesn’t happen through press releases or product brochures. It happens through stories that feel true because they are true.
What Real Stories Do That Product Videos Can’t
We’ve produced enough of both to know the difference. This is what we’ve seen.
Real stories transfer trust. When a physician watches a patient describe their experience in their own words, the trust that patient has earned transfers to the device. No amount of product footage or data slides can replicate that transfer. It’s human to human, mediated by a camera but not manufactured by one.
Real stories get shared. Product videos get watched when someone has to. Patient stories get shared when someone wants to. We’ve had physicians send our patient films to colleagues with a note that says, “Watch this.” That’s word-of-mouth at a level that paid distribution can’t buy.
Real stories last. A product demo becomes outdated when the next version ships. A patient story remains relevant for years because the human experience doesn’t have a version number. Paula’s story will be compelling as long as people experience knee pain. That’s a long time.
Real stories work across audiences. A product video is made for a specific viewer: the surgeon, the procurement officer, the clinical evaluator. A patient story works for all of them because the story is universal even if the clinical context is specific. The surgeon sees a patient they could treat. The procurement officer sees a life that changed. The evaluator sees evidence that the device works in the real world, not just in a controlled study.
Real stories align the organization. When your sales team, your marketing team, your clinical team, & your leadership all rally around the same patient story, something powerful happens. The organization stops talking about features & starts talking about impact. Internal meetings change. External conversations change. The story becomes the connective tissue that holds the message together across every touchpoint.
Why Most Medtech Companies Don’t Do This (Yet)
If real patient stories are this effective, why isn’t every medtech company doing it? We’ve asked ourselves that question a lot. This is what we’ve found.
Fear of losing control. When you put a real patient on camera, you can’t fully control what they say. That scares legal departments. It scares marketing teams used to message-controlled content. But the perceived risk is almost always greater than the actual risk. With proper pre-interviews, clear consent processes, & an experienced production team, patient stories can be both authentic & compliant. The key is preparation, not control.
The regulatory assumption. Many teams assume that FDA promotional guidelines make patient stories too risky. In practice, the guidelines are navigable if your production team understands them. A patient sharing their experience is different from a promotional claim. The line exists, & it can be walked with care.
The product-first reflex. Medtech companies are, by nature, engineering-driven. The instinct is to lead with the technology: how it works, what it does, why it’s superior. That instinct produces good spec sheets & mediocre videos. The best medtech video starts with the person, not the product. The product enters the story when it’s time, not before.
Not knowing where to find the stories. This is simpler than it seems. Your clinical team talks to patients every week. Your sales team hears outcomes in the field. Your customer service team gets calls from people whose lives changed. The stories are already happening. Someone just needs to capture them.
How to Start: The First Steps Toward Real Storytelling
You don’t need a massive production budget to start telling real stories. You need a commitment to finding them & the discipline to tell them well.
Start with a story audit. Ask your sales team, your clinical team, & your customer support team: who are the patients whose outcomes have been most striking? Make a list. Then have someone who knows how to listen, not sell, call those patients & have a conversation. You’re looking for natural storytellers with genuine, compelling outcomes.
Invest in pre-interviews. Before any camera rolls, spend time with potential subjects. Learn their story. Understand what matters to them. Find the moments that carry emotional weight. This step is where most productions succeed or fail, & it happens before a single piece of equipment leaves the truck.
Bring regulatory in early. Show your legal & regulatory team what you’re planning. Walk them through the interview approach. Address their concerns before production. When regulatory is a partner in the process, not a gatekeeper at the end, the work is better & the timeline is shorter.
Protect the story. This is our core belief at Beard & Bowler. Every production decision, from camera angle to music choice to edit structure, should serve the story. The story comes first. Brand, product, marketing calendar, all of it follows. When you protect the story, everything else follows. The brand benefits because the content is authentic. The product benefits because the story creates belief. The marketing calendar benefits because one strong story generates more usable content than a dozen scripted pieces.
The Moment That Proves It
There’s a moment in every patient story shoot that tells us whether we have something real. It usually happens about 20 minutes into the interview, when the subject forgets the camera is there. Their posture changes. Their voice drops. They stop performing & start remembering.
That’s when Paula told us about the morning she woke up without pain. That’s when Lea described the surprise of being clear-headed after surgery. That’s when the PKD siblings talked about what it means to face the same diagnosis as the person sitting next to you at Thanksgiving.
Those moments can’t be manufactured. But they can be found, protected, & shared with the people who need to see them.
That’s what happens when a medical device company tells a real story. Not a campaign. Not a content strategy. A story that’s true, told by the person who lived it, produced with the care it deserves.
If you’re ready to find those stories in your own organization, we should talk. You can also see examples of this work on our our work page, or read about building a video strategy that puts real stories at the center. For more about our approach, visit our services page or check the FAQ.
Frequently Asked Questions
How do you find patients willing to share their stories on camera?
It starts with your clinical & sales teams. They know which patients have had remarkable outcomes & are naturally vocal about their experiences. We then conduct pre-interviews to assess comfort on camera, storytelling ability, & the strength of their narrative arc. Most patients are honored to be asked. They want to help others who are going through what they went through. The key is approaching them with respect, not as marketing subjects but as people whose experience matters.
What if a patient’s story includes negative aspects or complications?
Authenticity means telling the full story, including the hard parts. A patient who describes their fear before surgery or the difficulty of recovery before the device helped them is more credible than one who only has positive things to say. The struggle makes the outcome meaningful. We guide the narrative to be honest without being gratuitous, & we work with your regulatory team to ensure everything stays within compliant boundaries.
How do real patient stories perform compared to traditional product videos?
Consistently better across every metric that matters. Higher completion rates, more shares, longer meeting times when used in sales, & stronger recall in follow-up conversations. The reason is simple: people remember people. A product spec fades from memory. A patient’s face & voice stay with you. The shift from brochures to video is accelerating for exactly this reason.
Can patient stories work for devices that treat less visible or dramatic conditions?
Yes. In fact, they often work even better. When a condition doesn’t have dramatic visual symptoms, the patient’s description of their experience becomes even more important. Living with chronic pain, fatigue, or a condition that others can’t see is deeply relatable. The story gives the invisible experience a face & a voice, which is exactly what makes it powerful in a sales or awareness context.
How long does it take to produce a patient story film?
From initial patient identification to final delivery, typically 6 to 10 weeks. That includes pre-interviews, production planning, a day of filming, post-production, & review cycles with your team. The timeline can be compressed for urgent needs, but we recommend giving the process room to breathe. Rushed patient stories feel rushed. The best ones take the time they need.